- August 29, 2018
- Gastroenterology
- Anna Mallaalieva
Currently, most people suffer from diseases of the gastrointestinal tract. The reasons that cause such problems are quite banal. First of all, this is poor nutrition and abuse of junk food. The drinks that fill store shelves most often contain various additives. They irritate the mucous membrane, which leads to malfunctions of the body and the development of such a stomach disease as focal gastritis. It is impossible not to mention bad habits. Smoking and drinking alcohol have a detrimental effect on the entire body. Also at risk are people living in constant stress.
It is worth noting that with stomach diseases, a person can neither fully work nor rest. Severe pain, heartburn, vomiting, and a persistent feeling of nausea become his constant companions. These symptoms indicate the development of gastritis. In medicine, there are several varieties of this disease. One of them is focal. Let's figure out what its peculiarity is and what complications it causes.
Focal gastritis - what is it?
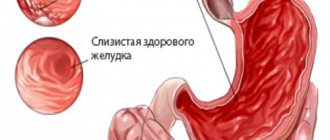
With this disease, the gastric mucosa becomes inflamed. Its characteristic difference is the formation of one or more foci. Their number may increase over time. People of different ages are at risk. At the initial stage, gastritis is accompanied by slight discomfort in the stomach and nausea. A little later, vomiting begins and pain appears. A disorder of the digestive system leads to disturbances in the gastrointestinal tract.
Based on the severity of the disease, doctors distinguish several varieties of this gastritis. Some of them are easily treatable, while others, on the contrary, can lead to the development of cancer if the correct therapeutic measures are not applied in time.
Description of the disease
Focal gastritis is an inflammation of the gastric mucosa, which is characterized by the appearance of lesions on the surface of the organ. This disease occurs quite often, and it is detected in people of any age. Stomach pathology is characterized by pain in the epigastrium, heartburn, nausea and vomiting. The number of lesions may vary.
Depending on the location of the lesion, the severity of the pathological process and the characteristics of the course, this gastritis is divided into several varieties. Thus, the catarrhal form of the disease can be easily cured, while atrophic gastritis can transform into cancer in the absence of adequate therapy.
Classification
So, let's look at the three main forms of this type of gastritis:
- Atrophic. With this form, a modification of the mucous membrane occurs. The functionality of the glands that produce pepsin decreases. This enzyme is involved in digestion. Inflammatory lesions show signs of atrophy. Epithelial tissue is formed. Due to the lack of pepsin, the stomach walls are further depleted.
- Non-atrophic. This form is characterized by the absence of epithelial tissue formation. The mucous membrane remains unchanged. The size of inflammatory areas may increase depending on the intensity of pathological changes. There are no signs of atrophy on the lesions.
- Chronic focal gastritis. The use of incorrect treatment methods in the acute form leads to the pathology moving into another phase. Doctors call it chronic. It is characterized by frequent relapses, during which symptoms similar to cancer are clearly expressed. With this form of gastritis, inflammation is sluggish. A slight modification of the mucous membrane is observed.
Causes
There are many reasons that can become a catalyst for the occurrence of focal forms of gastritis. Unfortunately, the life of a modern person is rarely complete without the use of medications, harmful products and any infectious diseases. All this has a destructive effect on the gastric mucosa and provokes its inflammation.
Causes of pathology:
- Use of chemicals.
Medicines, food flavorings and low-quality alcohol literally corrode the stomach tissue, which leads to the appearance of gastritis. Some people may ingest prohibited liquids, which also does not go unnoticed for the body.
- Failure to comply with nutritional rules.
Often, due to professional activities, a person does not have time to eat properly, preferring quick snacks. Also, a large amount of spices in the diet, fast food and fatty foods harms the stomach.
Such a habit as eating enough food once a day has a detrimental effect. The organ produces hydrochloric acid all day, destroying its own walls, then the person stretches the stomach with a large amount of food and then falls asleep, thereby starting rotting processes in the body.
- Accompanying illnesses.
Any infection or virus, as well as the presence in the body of other pathologies along the gastrointestinal tract, can provoke the occurrence of focal gastritis. Often, such patients have a history of food allergies, the presence of the Helicobacter pylori bacterium in the gastric juice, or any congenital defects of the digestive system.
Among the main causes of gastritis are autoimmune disorders, helminthic infestation, impaired metabolism or a hereditary predisposition to this pathology.
Erosive gastritis
Focal erosive gastritis is accompanied by very severe pain. They are caused by numerous lesions that affect the gastric mucosa. Patients often experience bleeding. This type of gastritis can be caused by Helicobacter pylori infection. In addition to it, there are other factors that cause this disease. These include:
- Long-term drug treatment with drugs that irritate the mucous membrane.
- Autoimmune disorders.
- Nervous disorders, stress.
- Problems of the endocrine system.
The disease occurs with pronounced symptoms:
- Pain syndrome in the upper abdomen. It can manifest itself either quite weakly or very strongly.
- With internal bleeding of varying degrees of intensity, the color of the stool changes. It acquires a characteristic black tint.
- Nausea, often accompanied by vomiting. In some cases, there is an admixture of blood in the vomit.
Medications
As practice shows, treatment of atrophic gastritis (reviews from doctors is proof of this) is a very lengthy process and does not always lead to satisfactory results. The main drug regimens for autoimmune atrophic inflammation of the gastric mucosa consist of three points:
- Etiotropic therapy . The stage is based on removing from the body the main cause of all gastritis, including this one - Helicobacter Pilory . For this, three or four-step therapy is used, which consists of drugs:
- an antibacterial drug (tetracycline or penicillin, as well as metronidazole in four-component therapy);
- a proton pump inhibitor drug (in this case it does not reduce acidity, but has a protective effect on the remaining healthy areas);
- bismuth preparations, which have a protective effect on the erosive surface of the mucosa and allow the restoration of the gastric mucosa.
- Increased acidity of gastric juice, resulting in improved digestion. They use drugs like Limontar , Abomin , Pepsidil and others.
- Drugs for the treatment of complications of chronic atrophic gastritis:
- improving peristalsis and advancement of chyme ( Motilium , Metoclopramide or Cerucal and others);
- antispasmodics to relieve possible pain syndrome ( Drotaverine or No-Shpa , Spazmalgon and others);
- correction of deficiency anemia using parenteral (usually intramuscular) administration of vitamin B12 , and with a high degree of anemia, sometimes they even resort to blood transfusions.
Catarrhal gastritis
The superficial form of gastritis, also known as catarrhal, develops very quickly. Literally a few hours after exposure to an aggressive substance on the mucous membrane, inflammatory foci form. This type of disease comes in two types: acute and with the development of focal atrophy.
Reasons for the development of acute catarrhal gastritis:
- Abuse of unhealthy street food.
- Frequent overeating.
- Bad habits (alcohol).
- Unbalanced diet.
- Unbalanced mental state.
- High physical activity.
Superficial gastritis with focal atrophy is expressed by disturbances in the functions of the stomach, in particular endocrine and motor functions. There is also a significant decrease in regenerative abilities. The symptoms are clear and manifested by the following factors:
- Intestinal disorders.
- Nausea that almost never stops.
- After eating, belching and heartburn occur.
- At the acute stage, there may be vomiting.
- Sharp weight loss.
- Pain in the upper abdomen.
- Autonomic dysfunction.
What it is?
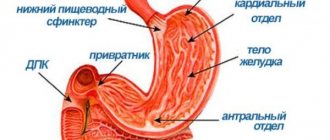
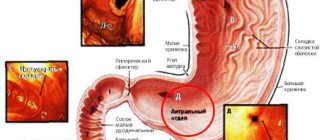
Antral gastritis (antrum gastritis) is a chronic inflammation of the gastric mucosa , leading to deformation of the pyloric (antral) part of the organ and disturbances in its motor function.
Source: dic.academic.ru
The focal form of antral gastritis refers to the initial manifestations of the disease. It is characterized by the presence of an inflammatory process in certain areas of the antrum of the stomach while maintaining the integrity of the submucosal layer and glands. Foci of epithelial atrophy may develop.
The reasons for the development of this type of gastritis may be as follows:
- The parasitic activity of the bacterium Helicobacter pylori, which provokes inflammation of the mucous membrane, disrupts its structure and increases the level of stomach acidity.
- Autoimmune processes in the body that suppress the normal functioning of the gastric mucosa and lead to a chronic course of the disease.
- Systematic eating disorders, food and alcohol poisoning, stress, bad habits.
Symptoms
At the initial stages of the development of the disease, the symptoms are not too pronounced : painful and dyspeptic manifestations are absent or episodic in nature, normal gastric acidity and satisfactory digestive function are preserved.
The progression of the disease gradually leads to a deterioration in a person’s well-being. A cramping pain appears in the upper abdomen an hour or two after eating, sour belching, a feeling of fullness in the stomach, vomiting, and diarrhea.
Don't self-medicate! At the first warning symptoms, seek advice from specialists.
Diagnostics
The goal of diagnosing gastritis is to accurately determine the causes or type of causative agent of the disease. The final diagnosis is made based on the results of laboratory tests and collected medical history. For gastritis, the following diagnostic measures are carried out:
- general and biochemical blood test;
- blood test for antibodies against Helicobacter pylori;
- respiratory test for the presence of Helicobacter pylori in exhaled air;
- determination of gastric juice acidity;
- stool analysis for helicobacteriosis.
The type of instrumental examination depends on the stage of the disease and can take the following forms:
- X-ray of the stomach;
- endogastroscopy or fibrogastroduodenoendoscopy (a study involving a biopsy - sampling of affected stomach cells for histology);
- electrogastrography (analysis of gastric motility).
Focal mucosal hyperplasia
Focal gastritis can occur with the formation of hyperplasia on the gastric mucosa. This complication is caused by increased cell growth. Most often, this pathology appears in the chronic form of the disease. There can be two types:
- Lymphofollicular. Occurs due to hormonal imbalances or secretory function disorders. The cells grow in the follicular layer of the gastric mucosa.
- Polypoid. This form is diagnosed in the presence of Helicobacter pylori infection that cannot be treated.
Causes of the disease
Various factors can provoke the development of the disease. Most often, the root cause of the disease is unhealthy eating habits:
- frequent consumption of fatty, spicy, fried foods;
- love of snacks and carbonated drinks;
- lack of hot broths in the diet;
- long breaks in nutrition;
- food dry and on the go;
- non-compliance with drinking regime.
Alcohol and certain medications are considered a negative irritant to the gastric mucosa. Indirect factors that can cause focal superficial gastritis are recognized:
- duodenogastric reflux is a pathology when the contents of the duodenum are released into the stomach;
- stress;
- tendency to allergies;
- smoking;
- cases of gastritis in the family;
- chemical and radiation exposure;
- difficult working conditions;
- individual predisposition.
The most common causative agent of the disease is the bacterium Helicobacter pylori. A complication of a number of diseases (high blood pressure, heart and liver dysfunction, diabetes mellitus, hormonal imbalance) is the development of gastritis.
Diagnostics
Focal gastritis is accompanied by symptoms that are similar to those of other stomach diseases, so it is very important to make a correct diagnosis. For this reason, doctors prescribe a number of laboratory tests.
- Stool analysis. Carrying out a scatological examination allows you to accurately determine the source of inflammation and identify internal bleeding.
- General blood analysis. Doctors pay attention to the number of white blood cells. Their hanging indicates an inflammatory process. Gastritis is also indicated by a decrease in hemoglobin.
- Blood test (ELISA). Allows you to detect the presence of Helicobacter pylori in the body, in particular in the stomach or duodenum.
- Breath test. If a concentration of ammonia is felt when exhaling, this indicates that the stomach is infected with the spiral-shaped bacterium Helicobacter pylori.
- Endoscopic examination. Used to visually determine the condition of the mucous layer and walls of the stomach. If oncology is suspected, during such a study a biopsy is taken for histology.
Diagnosis of the disease
To make an accurate diagnosis, the patient needs to undergo several instrumental examinations and pass all the tests prescribed by the doctor. For focal gastritis, it is most often recommended:
- general blood test - helps to find indirect signs of gastritis to prescribe further examinations,
- coprogram - studying the composition of stool helps to separate stomach diseases from diseases of the liver and pancreas,
- breath test - prescribed to determine Helicobacter pylori,
- ELISA analysis is an accurate method for determining bacteria in the body,
- FGDS is an endoscopic procedure with which the doctor visually assesses the condition of the stomach and mucous membrane.
In the process of FGDS, gastric tissue is often collected for subsequent histological analysis.
Focal gastritis: treatment
Patients who have already been diagnosed need treatment. It includes not only taking medications, but also a special diet, as well as physical procedures. Positive results can be achieved by strictly following all instructions. Only patients with acute forms of gastritis require hospitalization; for chronic cases, it is necessary to regularly visit a gastroenterologist.
How is drug treatment carried out?
- If Helicobacter pylori is detected, the patient is prescribed antibacterial drugs. After using them, you need to take medications that restore the microflora.
- If gastritis occurs with increased acidity, then it is necessary to take antisecretory drugs and histamine blockers.
- To speed up digestion, prokinetics are prescribed.
- If inflammation of the gastric mucosa causes disruption of the endocrine system, doctors prescribe a course of pancreatin.
- Taking antacids can relieve heartburn, reduce acidity and protect the affected areas of the mucous membrane.
- Antispasmodics are prescribed to reduce pain.
Treatment
Treatment of focal gastritis includes several main stages. The patient must take several groups of medications that help protect the stomach and eliminate symptoms.
In addition, the stomach is put into a gentle mode of operation, trying not to injure the walls of the organ with rough food. After a couple of weeks of such treatment, physiotherapy can be added to the main therapy.
How to cure focal gastritis:
- Medicines.
Antacid medications are required to protect the gastric mucosa. Prokinetics or proton pump blockers are prescribed to correct hydrochloric acid levels, if required.
To improve digestion, taking enzymes, vitamin complexes and beneficial bacteria is recommended. Pain can be relieved with antispasmodics, which are taken as needed. Drug therapy forms the basis of all treatment; without the use of medications, stomach inflammation cannot be cured.
- Diet.
Attention must be paid to a special therapeutic diet. The diet should exclude all foods that can injure irritated stomach tissue. The patient is advised to avoid fried foods, rough vegetables and raw fruits, whole grain cereals, and carbonated drinks.
Alcohol and smoking are mandatory. Food should not be too hot or, conversely, cold, or contain a lot of sauce, vinegar or spices. You need to stay in this mode for at least 2 weeks, after which you can gradually introduce your usual dishes.
With a single episode of gastritis, a person should completely reconsider his diet, making a bias in food in favor of healthy foods.
- Spa treatment.
To completely get rid of the consequences of focal gastritis, you can visit a medical sanatorium. There, the patient will be taught how to eat properly, and will also undergo a number of useful physical procedures to restore the body.
Systematic intake of table mineral water has a good therapeutic effect. Treatment in a sanatorium will help get rid of residual manifestations of the disease and achieve stable remission.
Diet
Focal gastritis cannot be cured unless you adhere to a diet. It is prescribed only by a gastroenterologist. What should a sick person not eat?
- Carbonated drinks.
- Juices with preservatives.
- Any food that contains dyes and various additives.
- Rough products such as nuts, white cabbage, bran and others.
- Fatty, salty, spicy foods.
For low acidity, it is recommended to take freshly squeezed vegetable and fruit juices, decoctions of grapes and rose hips. If gastritis is accompanied by high acidity, then the daily diet consists of dishes such as cereals, soups and jelly. You can only eat lean meat, dairy products and boiled vegetables.
During the diet, it is important to adhere to a strict daily routine. Meals are taken by the hour.
Preventive actions
Methods for preventing the disease include maintaining a healthy lifestyle. It is important to take into account negative influence factors, such as harmful production, smoking and drinking alcohol, unhealthy diet and lack of eating habits. Abuse of these conditions can provoke an exacerbation of an old disease or become a prerequisite for the formation of a new one.
https://www.youtube.com/watch?v=HnQRGC4xd9s
It should be taken into account that chronic focal gastritis can develop under the influence of other painful conditions. For these purposes, it is recommended to systematically undergo examinations to detect helminthiases, chronic diseases of the liver, pancreas and intestinal infections. It is recommended to avoid situations that may provoke an increase in intra-abdominal pressure. These include intense physical activity, bloating, constipation, and tightly tightened belts.
For preventive purposes, you should undergo sanatorium-resort treatment; drinking mineral waters is especially useful. As a rule, doctors prescribe for patients with high acidity levels to visit resorts with sources of alkaline water. For low stomach acidity, salt and salt-alkaline waters are recommended.
It is not the components of mineral water that play an important role, but the time of its consumption. During the hyperacid stage, you should drink water several hours after eating. A good preventive measure would be treatment with mineral water at home. To do this, you need to consult with your doctor, who will prescribe a water intake regimen. Typically, such treatment is carried out 1-2 times a year, and the course duration is up to 6 weeks.
https://www.youtube.com/watch?v=3ZkiLw1lC5I
You should not select medications for yourself, but you can read the overview and indications of medications. Be sure to always re-read the recommendations indicating compliance with the rules. This will avoid complications and prevent the worsening of the painful condition. If you have chronic focal gastritis, it is recommended to undergo regular examinations and be under medical supervision.
These measures are necessary because this will help in the future to prevent the risk of degeneration of inflammatory processes into a more serious disease.
Reasons for the development of gastritis
The formation of focal gastritis is caused by many reasons, including activation of the bacterium Helicobacter pylori. However, it is necessary to distinguish causes from provoking factors:
- a sharp decrease in immunity - occurs against the background of sluggish infectious and inflammatory processes, as well as due to other diseases;
- taking medications without the consent of a doctor - incorrect dosages and regimen of medications can lead to the development of the disease;
- gross violation of nutritional rules - a huge amount of store-bought products, fatty and spicy foods leads to illness. Overeating, late dinners, and improper nutrition can also trigger gastritis;
- drinking alcohol in large doses - alcohol irritates the mucous membrane and leads to its thinning over time;
- constant stress - nervous overstrain provokes various diseases, and focal gastritis cannot be considered an exception.
Other pathologies can lead to the formation of foveal focal gastritis: diabetes, metabolic disorders, heredity, endocrine disorders, weak immunity and autoimmune diseases. The age group should be highlighted separately - people over 60 years of age are especially susceptible to stomach diseases.
Symptoms
Uncomplicated forms of gastritis are accompanied by discomfort, a burning sensation, and heaviness in the epigastric region after eating. Often the patient notices belching and severe nausea. When areas of hyperplasia of the gastric mucosa expand, the following symptoms develop:
- loss of appetite;
- smell from the mouth;
- coating on the tongue is white or gray;
- heartburn;
- vomit;
- milk intolerance;
- strong pain;
- bloating;
- weight loss;
- general weakness;
- low-grade fever.
Clinically, there are several types of focal gastritis, which differ from each other in the nature of damage to the gastric mucosa, as well as in location:
- Chronic focal gastritis. The chronic form of the disease with focal atrophy is characterized by an unexpressed process of inflammation, minor changes in areas of epithelial tissue, and rare exacerbations that usually occur in the off-season, against the background of other diseases of the digestive tract.
- Focal atrophic gastritis. It is characterized by pronounced atrophy of the mucous membrane, accompanied by a decrease in the secretion of pepsin, the acidity of gastric juice and impaired digestion of food. This form of the disease subsequently leads to thinning of the mucosa.
- Non-atrophic gastritis. This type of pathology does not lead to a decrease in the density of the gastric mucosa, but causes foci of severe inflammation. The depth of the lesion is determined by the intensity, duration and cause. The prognosis with timely treatment of the non-atrophic type of gastritis and in the absence of concomitant chronic diseases of the gastrointestinal tract is usually favorable.
- Superficial focal gastritis. This type of pathology is more common than others, and it is more treatable due to the fact that the mucous membrane is not significantly damaged. Focal catarrhal gastritis is manifested by minor discomfort immediately after eating.